|
Getting your Trinity Audio player ready...
|
Have you ever heard of pterygium? It’s a common eye condition that affects millions of people worldwide.
If you’re not familiar with it, you’re not alone.
Pterygium is often overlooked or misunderstood, but it’s important to raise awareness about this condition and its potential impact on vision.
Pterygium can lead to discomfort, vision problems, and potential complications if left untreated.
Introduction
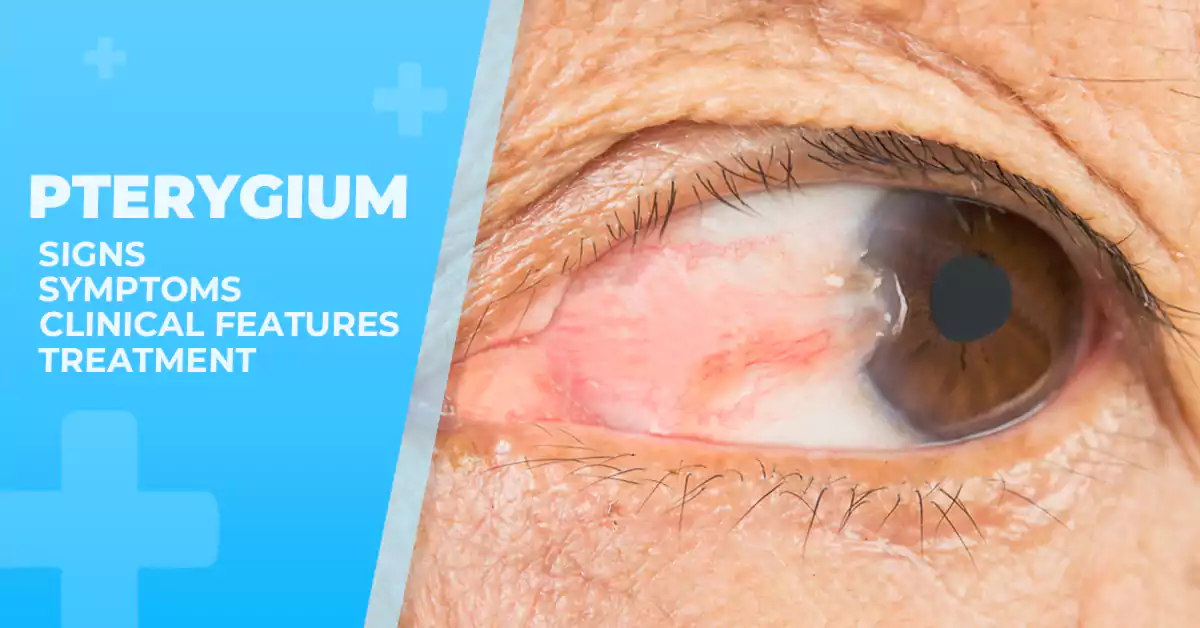
Pterygium, pronounced as “ter-ij-ee-um,” is an abnormal growth of tissue on the surface often referred to as “surfer’s eye” due to its association with outdoor activities of the eye.
It is typically triangular-shaped forming on the conjunctiva, the clear tissue that covers the white part of the eye.
It starts as a small, pinkish bump and can gradually grow over time, causing various symptoms and complications if left untreated.
Your eyes may be red, swollen, and irritated in mild cases.
If the pterygium grows, your vision may be blocked or blurred.
In this comprehensive article, we will explore what pterygium is, its causes, symptoms, and the available treatment options.
What is pterygium?
Pterygium is a non-cancerous growth of tissue on the conjunctiva, the thin, transparent membrane that covers the white part of the eye (sclera) and the inner surface of the eyelids.
It usually begins on the side of the eye nearest the nose and gradually extends toward the cornea—the clear, dome-shaped outer layer of the eye.
Symptoms of Pterygium:
Pterygium can vary in severity, and some individuals may not experience any symptoms. However, when symptoms do occur, they may include:
- Redness and Inflammation: The affected eye may appear red and inflamed due to the presence of the pterygium.
- Irritation and Discomfort: Pterygium can cause a persistent feeling of irritation or grittiness in the eye.
- Foreign Body Sensation: Individuals may experience the sensation of having a foreign object in the eye.
- Blurred Vision: When the pterygium becomes large enough to cover the cornea, it may cause vision to become distorted or blurred.
- Dryness and Tearing: Pterygium may disrupt the normal tear film, leading to dry eyes or excessive tearing.
Causes of Pterygium:
The exact cause of pterygium is not fully understood, but several factors contribute to its development:
- Excessive UV Exposure: Long-term exposure to ultraviolet (Ultraviolet light) radiation from the sun is considered the primary risk factor for pterygium, making it more prevalent in individuals living in sunny climates or those with frequent outdoor activities.
- Dry and Dusty Environments: People exposed to dry, dusty, and windy conditions are at an increased risk of developing pterygium, as environmental irritants may trigger its formation.
- Genetics: Some studies suggest that genetics may play a role in pterygium development, as it tends to run in families.
- Chronic Eye Irritation: Constant eye irritation from factors like pollution, allergens, or contact lenses can contribute to the development of pterygium.
Diagnosis of Pterygium
Diagnosis of pterygium is typically made during a comprehensive eye examination, which may include a slit-lamp examination to assess the extent of the growth and its impact on the cornea.
The presence of blood vessels, corneal topography changes, and corneal opacity are key factors that aid in the diagnosis.
Early diagnosis and management of pterygium are crucial to prevent further progression and potential loss of vision.
Slit-lamp Examination
The slit-lamp examination is a crucial diagnostic tool used to evaluate and diagnose pterygium.
During this examination, the ophthalmologist or eye specialist examines the eyes using a slit-lamp microscope to assess the location, size, vascularity, and extent of the pterygium.
To perform the examination, the patient is asked to sit at the slit-lamp microscope while the doctor applies topical anesthetic eye drops for comfort.
The doctor then uses the slit-lamp microscope with a high-intensity light beam and a thin, slit-shaped light source to focus on the pterygium.
Oblique illumination is used to assess the location and size of the pterygium.
The doctor examines the eye and determines whether the pterygium is located on the nasal or temporal side of the eye.
Using Castroviejo’s calipers, the size and length of the pterygium are measured.
Vascularity is assessed by examining the blood vessels on the surface of the pterygium.
The doctor observes the intensity, density, and tortuosity of the blood vessels.
This information helps determine the severity of the condition and guide treatment decisions.
In addition to location, size, and vascularity, the examination also involves assessing the extent of the pterygium and its involvement with the cornea.
The doctor carefully examines the pterygium’s advancement onto the cornea and monitors for any signs of corneal involvement, such as changes in corneal transparency or irregular astigmatism.
It is important for the doctor to note the presence or absence of Stocker’s line, which appears as a thin, gray line on the corneal surface.
The presence of Stocker’s line suggests chronic irritation and inflammation caused by the pterygium.
Overall, the slit-lamp examination is a valuable tool for evaluating and diagnosing pterygium.
It allows the doctor to assess the location, size, vascularity, and extent of the pterygium, as well as note any corneal involvement or the presence of Stocker’s line.
This information helps in developing an effective treatment plan for patients with pterygium.
Visual Acuity and Blurred Vision Tests
Visual acuity and blurred vision tests play a crucial role in assessing the severity and impact of pterygium, a condition characterized by the growth of tissue on the bulbar conjunctiva.
These tests evaluate the patient’s ability to see clearly and focus on objects.
The most commonly used test is the Snellen chart, which measures visual acuity.
Patients are asked to read letters or numbers on the chart from a distance of 20 feet.
The results are recorded as a fraction, with the numerator representing the distance at which the patient stands compared to the denominator, which represents the distance at which a person with normal vision would see the same line.
Other visual acuity tests include visual acuity charts, which are similar to Snellen charts but can be used at a close distance, and astigmatism tests, which assess the patient’s ability to focus on objects at different distances and in different directions.
In addition to these standard tests, specialized techniques like corneal topography can be used to measure the shape and curvature of the cornea, which can be affected by pterygium.
This can provide valuable information about the impact of the growth on the patient’s vision and guide the appropriate treatment approach.
By conducting these visual acuity and blurred vision tests, healthcare professionals can accurately assess the extent of pterygium and determine the best course of action for each patient.
Other Tests for Symptom Assessment
In addition to visual acuity and blurred vision tests, there are several other tests used for assessing symptoms of pterygium.
These tests help to diagnose and evaluate the severity of the condition.
One such test is a slit-lamp examination, which allows the healthcare professional to closely examine the pterygium and its impact on the surrounding structures.
This test helps to determine the size, shape, and extent of the pterygium, as well as any associated complications such as corneal opacity or scarring.
Another useful test is corneal topography, which measures the shape and curvature of the cornea.
This test can help identify any irregularities or changes in the cornea caused by the pterygium, which may contribute to blurry vision.
Additionally, a thorough evaluation of the patient’s medical history and risk factors is important.
Exposure to ultraviolet radiation and chronic eye irritation are common risk factors for developing pterygium and asking about these factors can help in diagnosing and managing the condition.
Overall, these tests and assessments play a crucial role in diagnosing pterygium and determining its severity.
By understanding the extent of the pterygium and its impact on visual function, healthcare professionals can formulate a treatment plan tailored to the specific needs of each patient.
Treatment Options for Pterygium:
The management of pterygium depends on the severity of symptoms and the risk of vision impairment. Some treatment options include:
- Conservative Management: Mild pterygium with minimal symptoms can often be managed with lubricating eye drops to relieve dryness and irritation. Wearing protective sunglasses that block UV radiation can also help prevent further growth.
- Medications: In some cases, your eye doctor may prescribe anti-inflammatory eye drops to reduce redness and inflammation.
- Surgical Removal: If the pterygium causes significant discomfort, vision problems, or cosmetic reasons, surgical removal of pterygium may be recommended. The pterygium surgery typically involves excising the abnormal tissue and transplanting healthy conjunctival tissue to prevent recurrence.
- Amniotic Membrane Grafting: In more advanced cases or cases with a high risk of recurrence, amniotic membrane grafting may be used in combination with surgery to promote healing and reduce inflammation.
Non-Surgical Treatment Options
When it comes to managing pterygium, non-surgical treatment options are available for patients who want to avoid or delay surgical intervention.
These treatments aim to reduce inflammation, relieve symptoms, and prevent the growth or recurrence of the pterygium.
One of the first-line non-surgical treatments for pterygium is the use of lubricating eye drops or ointments.
These can help reduce redness, irritation, and dryness associated with the condition.
Lubricating eye drops works by providing moisture to the affected area and alleviating discomfort.
In some cases, anti-inflammatory eye drops may be prescribed to help reduce inflammation caused by pterygium.
These medications can help relieve symptoms such as redness, discomfort, and blurry vision.
However, it is important to note that anti-inflammatory eye drops are not commonly used and are reserved for rare cases.
In certain situations, other non-surgical treatments may be considered to prevent recurrences.
Surface radiation, conjunctival implants, or chemotherapy medications can be utilized to inhibit the growth or regrowth of the pterygium.
These treatments work by targeting abnormal blood vessels and preventing them from proliferating.
It is important to consult with an eye care specialist to determine the most suitable treatment approach based on the individual’s clinical presentation and specific needs.
They can assess the severity of the pterygium and recommend the appropriate non-surgical treatment options to manage the condition effectively.
Preventing Pterygium:
While it may not be possible to completely prevent pterygium, certain measures can significantly reduce the risk:
- Wear Sunglasses: Always wear UV-protective sunglasses when outdoors, especially in sunny or high-glare environments.
- Eye Protection: Use safety goggles or protective eyewear in dusty or windy conditions.
- Take Breaks: If your work involves prolonged screen time or eye strain, take regular breaks to rest your eyes.
- Avoid Irritants: Minimize exposure to irritants that could cause chronic eye irritation.
Conclusion:
Pterygium is a common eye condition associated with UV exposure and environmental factors.
While it may cause discomfort and vision problems, early detection and appropriate management can prevent complications.
If you experience any symptoms or notice abnormal growth in your eye, consult an eye care professional for a thorough evaluation and personalized treatment plan.
By taking preventive measures and seeking timely care, you can protect your eyes and maintain good ocular health for years to come.